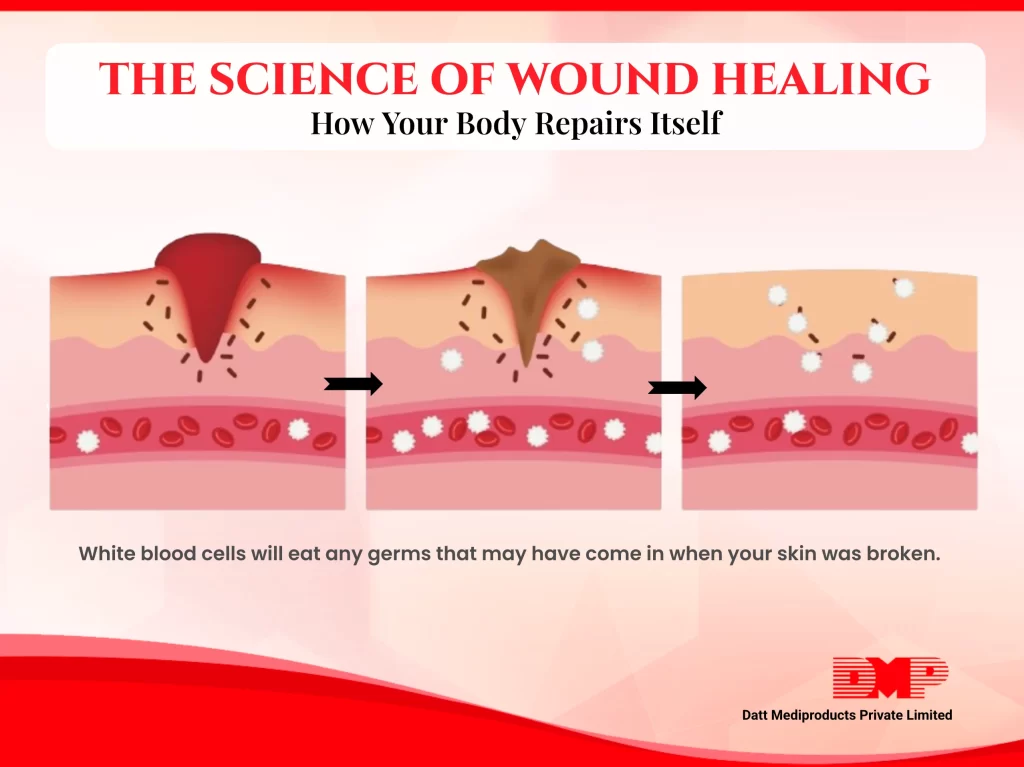
The microbes are ubiquitous and are found in water, air and soil. The fact is that not all microbes or germs are harmful, but some of them are good as well. The microbes cause illness only when they enter the part of the body where they are not supposed to be.
Thank God we are blessed with a defence system –immune system, which acts as a barrier against these germs, but surpassing this immune barrier causes infections.
Infections can be classified into four main categories based on their causative agent:
Bacterial, Viral, Fungal and Parasitic.
– Bacterial Infection:
Bacteria enter the body through the openings like mouth and nose, as well as cuts, scrapes, and even surgical incisions. Infection may also be transmitted by sharing towels, razors or spoons.
Bacteria are both ‘Bad’ and ‘Good’ and should not blame them for being around.
There are some ‘Bad Bacteria’ that are responsible for a number of diseases like Cholera (Vibrio cholerae), Tetanus (Clostridium tetani), Botulism (Clostridium botulinum) and many more.
Our body is habitat for some ‘Good Bacteria’ too that reside in our gut. These help our body in food digestion, nutrients absorption and production of several vitamins including folic acid, niacin, and Vitamins B6 and B12.
Whenever we encounter any bacterial infection we usually take antibiotics and these are supposed to be really effective in eliminating the infection. But many a times these antibiotics disturb the microflora present in the body and kill the helpful bacteria also. This creates imbalance of bacteria in the body leading diarrhea and other gastrointestinal problems.
The real threat to humans is the overuse and misuse of antibiotics as it leads to Antimicrobial resistance (AMR). The antibiotics are losing effectiveness as the bacteria are cleverly mutating, gaining resistance and becoming superbugs.
– Viral Infections:
Viruses are responsible for a wide range of infectious diseases like AIDS, Hepatitis, Flu, Covid 19 and many more.
Like bacteria they also enter the body through the openings like nose and mouth. They also spread through body fluids like contaminated blood and sexual activity.
Antibiotics are effective against only bacteria and the viral infections can be dealt with vaccines and antivirals. To prevent viral infections vaccines are administered timely since birth and thereafter after regular intervals. Many of the vaccines require booster doses for life-long immunity.
– Fungal Infections:
The fungal infections are generally harmless but more annoying. These infections may appear on any part of the body from ringworm of the scalp, athlete’s foot in between the toes, vaginal yeast infection in women are few of them.
Fungal spores are found on dead, decayed and rotten vegetation. Inhaling fungal spores is one of the most common ways to develop an internal fungal infection.
The fungal infection can be treated by specific anti-fungal medications. These can be in the form of cream or ointment, suppository, or pill form.
– Parasitic Infections:
Parasitic infections like malaria, are the most common and are spread are spread through the bites of infected mosquitoes.. Other infections include Chagas disease, Cysticercosis (by tapeworm), Trichomoniasis (a sexually transmitted infection).
The presence of parasite can be easily detected with the help of blood, or stool test. The treatment of the parasitic infections depends on the type of infection and how far the infection has progressed.
Ways to Prevent
Primarily follow all the habits what we were doing for the past two years to keep the infection away
- Wash hands with soap and water often
- If water is not available use hand sanitizers instead
- Maintain personal hygiene
- Practice cough and sneeze etiquette
- Oral hygiene is crucial to keep gut infections at bay
- Keep immunization on records
- Practice safe sex
- Keep body dry and clean and wear breathable clothes to combat fungal infection
Study published by Centers for Disease Control and Prevention (CDC) suggests that washing hands regularly reduces Diarrhea infection by 23-40%.
Cancer patients bear risk of infection as they have compromised immune system due to medication and disease. They should monitor the signs and symptoms of infection and talk to the doctor immediately.
We @DattMediproducts suggest that infections should be taken seriously and seek medical advice before it worsens.
Follow the above healthy habits and stay safe.