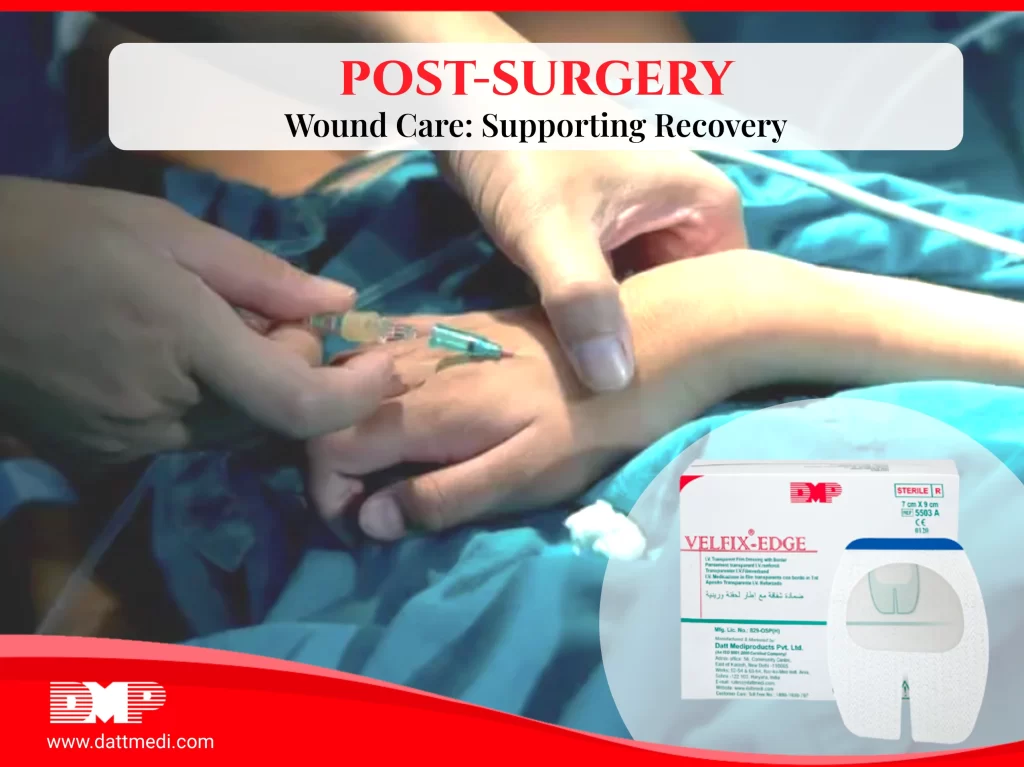
Post-Surgery Wound Care Supporting Recovery
Post-surgery wound care is a critical component in the journey towards a smooth recovery, minimizing complications, and promoting effective healing. This blog post seeks to offer comprehensive insights for both patients and healthcare providers, emphasizing key aspects of post-surgery wound care.
Understanding the Healing Process:
To navigate the recovery journey successfully, it’s essential to grasp the intricacies of the body’s natural healing process. From the initial inflammatory response to tissue remodeling, patients should be aware of these stages to set realistic expectations for the recovery timeline.
Preparation Before Surgery:
A proactive approach to wound care begins before the surgical procedure. Adequate preparation involves thorough consultation with healthcare professionals, understanding the surgery specifics, and adhering to pre-surgery instructions. This groundwork sets the stage for a more seamless recovery.
Maintaining a Sterile Environment:
Fundamental to effective wound care is the maintenance of a clean and sterile environment. This includes keeping the surgical site and surrounding areas free from contaminants. Proper wound hygiene significantly reduces the risk of infections, a common concern post-surgery.
Nutrition and Hydration for Optimal Healing:
Supporting the body’s healing mechanisms requires a well-balanced diet rich in essential nutrients. Proper nutrition promotes tissue repair and helps prevent complications. Adequate hydration is equally crucial, supporting overall bodily functions and facilitating nutrient transportation to the wound site.
Monitoring and Recognizing Warning Signs:
Vigilance is key during the recovery phase. Patients should be educated on monitoring wounds for warning signs like increased redness, swelling, or discharge.
Recognizing these signs early enables prompt intervention, minimizing the risk of serious complications.
Introducing Our Innovative Solution:
Elevating the standards of patient recovery involves introducing innovative products like Velfix® -Edge. This exceptional dressing goes beyond traditional solutions with its non-woven bordered design, frame delivery system, and deep notched barrier against infections. The latex-free adhesive ensures compatibility with diverse patients, while the window-framed delivery system simplifies application. Incorporating Velfix® -Edge into post-surgery wound care routines prioritizes precision, patient comfort, and infection prevention, contributing to an enhanced and smoother recovery journey for every patient.
Therefore, post-surgery wound care is a collaborative effort between healthcare providers and patients. Empowering individuals with knowledge about the healing process, preparing adequately before surgery, maintaining a sterile environment, prioritizing nutrition and hydration, and being vigilant for warning signs actively contribute to a successful recovery journey.
Choosing Velfix® -Edge for optimal post-surgery care is a conscious decision towards improved recovery outcomes, ensuring a holistic and effective approach to the healing process.