Absorbent foam dressings are advanced wound care solutions specifically designed to manage moderate to heavy wound exudate while maintaining a moist healing environment.
Maintaining the right moisture balance is critical for wound healing. Excess fluid can cause maceration and delay recovery, while insufficient moisture may slow tissue regeneration. Foam dressings are engineered to maintain this balance—supporting safer, more efficient healing across acute and chronic wound types.
Widely used in hospitals, long-term care facilities, and home-care settings, absorbent foam dressings are a core component of modern wound management protocols.
Clinical Overview: Absorbent Foam Dressings
- Designed for moderate to heavy exudate
- Maintain a controlled moist wound environment
- Reduce risk of periwound maceration
- Provide cushioning and mechanical protection
- Support atraumatic dressing removal
- Suitable for pressure ulcers, diabetic foot ulcers, venous leg ulcers, and surgical wounds
What Are Absorbent Foam Dressings?
Absorbent foam dressings are multi-layer wound dressings typically made from polyurethane foam. They are engineered to:
- Absorb and retain moderate to heavy wound fluid
- Protect surrounding skin from excess moisture
- Provide thermal insulation and cushioning
- Maintain optimal moisture levels for tissue repair
They are widely used in advanced wound care settings where effective exudate control and periwound protection are essential.
Why foam dressings are used
Wounds that produce fluid need balance—not dryness, not pooling moisture. Foam dressings maintain this balance, which supports natural tissue repair.
How they are built
- A highly absorbent foam layer that draws in and holds wound fluid
- A protective outer layer that allows airflow but blocks bacteria and external moisture
- Optional adhesive borders for secure placement without extra fixation
Foam dressings are widely used in acute care, long-term wound management, and post-surgical recovery across global healthcare systems, especially in wound care settings.
How Absorbent Foam Dressings Work
1. Managing Moderate to Heavy Wound Exudate
Foam dressings absorb excess fluid and lock it inside the dressing.
Why this matters:
Uncontrolled fluid can soften surrounding skin, increase leakage, and slow healing.
How it helps healing:
By keeping the wound surface balanced—not wet, not dry—foam dressings create conditions where new tissue forms more efficiently. Products such as Velnext® Foam Dressing are designed for this purpose.
2. Maintaining a Stable Healing Environment
While absorbing excess fluid, foam dressings preserve gentle moisture at the wound surface.
Clinical benefit:
Stable moisture supports faster cell growth and reduces repeated tissue disruption caused by frequent dressing changes, which is especially important in chronic wounds managed with advanced foam dressings
3. Cushioning and Physical Protection
The soft foam structure absorbs pressure and reduces friction.
Especially useful for:
- Heels
- Sacral area
- Elbows
- Other pressure-prone or mobile body parts
This protection helps prevent further tissue damage during daily movement and is a key benefit of foam-based wound dressings.

Read More about : VELFIX-S: Foam Dressings in Wound Care
Key Benefits of Absorbent Foam Dressings
Protects Periwound Skin
By preventing fluid leakage and excessive moisture accumulation, foam dressings reduce the risk of maceration and surrounding skin breakdown.
Enhances Patient Comfort
The flexible, conformable structure minimizes pain during wear and dressing removal, especially in chronic wound management.
Reduces Dressing Change Frequency
Due to their high absorbency, foam dressings can often remain in place for several days (subject to clinical assessment), improving patient compliance and care efficiency.
Supports Infection Management
In wounds with elevated infection risk, antimicrobial silver foam dressings may help manage bacterial load. These are typically used when clinical signs of infection are present or when risk factors exist.
Types of Absorbent Foam Dressings
Adhesive Foam Dressings
- Integrated fixation border
- Easy application
- Suitable for ambulatory patients and post-operative care
Non-Adhesive Foam Dressings
- Gentle on fragile or sensitive skin
- Require secondary fixation
- Ideal for elderly patients or delicate wound sites
Antimicrobial Foam Dressings
- Contain antimicrobial agents
- Support bacterial load management
- Used in infected or high-risk wounds
Foam Dressings vs Other Dressing Types
| Dressing Type | Best For | Not Suitable For |
| Foam Dressings | Moderate–heavy exudate | Dry wounds |
| Hydrocolloids | Light–moderate exudate | Heavily exuding wounds |
| Alginates | Heavy exudate or bleeding | Dry wounds |
| Transparent Films | Superficial wounds | Moderate–heavy exudate |
Selecting the appropriate dressing depends on wound characteristics, fluid level, and clinical assessment.
Ideal Wound Types for Foam Dressings
Absorbent foam dressings are commonly recommended for:
- Pressure ulcers
- Diabetic foot ulcers
- Venous leg ulcers
- Post-surgical wounds
- Traumatic injuries
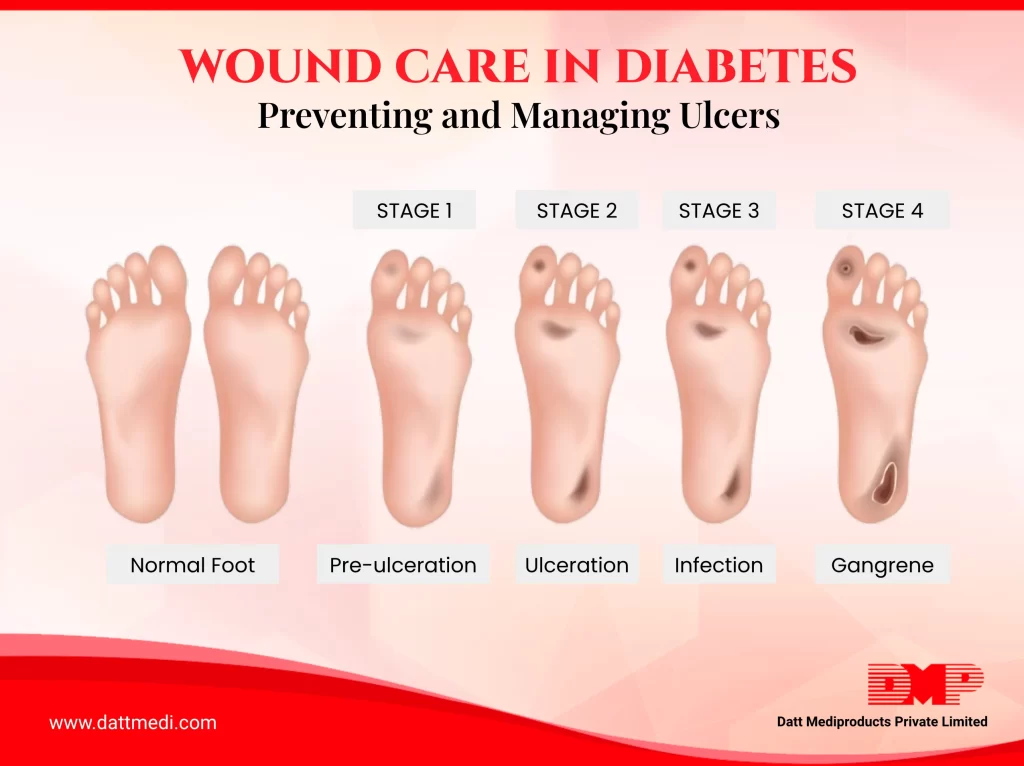
Read More: Proven Ways to Prevent Complications
Their ability to absorb fluid while protecting tissue makes them a reliable option for both acute and chronic wound care, including hospital-grade wound management.
When Foam Dressings May Not Be Appropriate
Foam dressings may not be suitable for:
- Dry or minimally exuding wounds
- Hard necrotic tissue or dry scabs
- Wounds requiring active debridement
In such cases, alternative dressing categories that donate moisture or facilitate debridement may be more appropriate based on professional evaluation.
Quality Standards and Clinical Reliability
High-performance absorbent foam dressings are manufactured in accordance with internationally recognized quality and safety standards, including ISO 13485 and CE certification.
As a manufacturer of certified advanced wound care solutions, DMP designs foam dressings aligned with global clinical standards, ensuring product reliability, patient safety, and consistent performance across healthcare environments.
Absorbent foam dressings combine smart material design with practical wound care needs. By controlling wound fluid, protecting fragile skin, and improving comfort, they play a vital role in modern wound management.
Selecting the right foam dressing—based on wound type, fluid level, and patient needs—can significantly improve healing outcomes and overall care quality.




