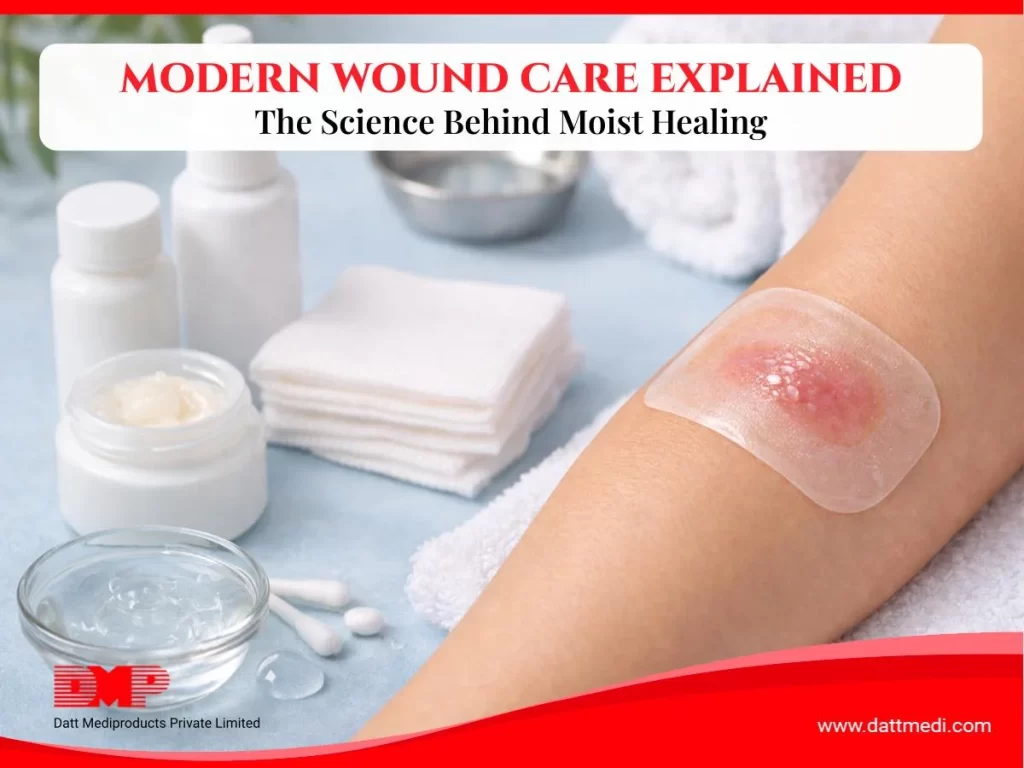
For many years, people believed that allowing a wound to dry out and form a scab was the best way to promote healing. Modern wound care science has shown that maintaining a moist healing environment can support faster tissue repair, reduce discomfort, and improve skin recovery.
Since its clinical adoption in the 1960s, moist wound healing has become a cornerstone of modern wound care in hospitals and home care settings worldwide. By protecting the wound and supporting the body’s natural repair process, this method helps improve healing outcomes and patient comfort.
What Is Moist Wound Healing?
Moist wound healing involves covering a wound with an advanced wound care dressing that maintains optimal moisture while protecting it from contaminants and bacteria.
Dry Healing Approach
- Allows a hard scab to form
- Can slow skin cell movement
- May delay tissue repair
Moist Healing Approach
- Keeps the wound hydrated
- Enables faster cell migration
- Supports efficient tissue regeneration
This balanced environment helps the body heal more effectively.
Moist Wound Healing vs Dry Healing: Key Differences
| Feature | Moist Healing | Dry Healing |
| Healing Speed | Faster | Slower |
| Pain Level | Reduced | Often higher |
| Infection Protection | Barrier protection | Exposure risk |
| Scarring | Less visible | More likely |
| Tissue Repair | Continuous | Interrupted by scab |
Why Moist Wound Healing Is Beneficial
1. Faster Healing
A moist environment allows skin cells to move easily across the wound surface.
- No hard scab blocking repair
- Continuous tissue rebuilding
- Shorter recovery time
This is especially beneficial for surgical wounds, burns, and chronic ulcers.
2. Reduced Pain and Discomfort
Dry wounds can expose nerve endings, increasing sensitivity and pain.
Moist dressings:
- Protect delicate tissue
- Reduce irritation
- Provide cushioning comfort
They are commonly used to soothe painful wounds and burns.
3. Lower Risk of Infection
Advanced wound dressings create a protective barrier against dirt and bacteria.
When combined with antimicrobial protection, they:
- Reduce contamination risk
- Support safer healing
- Assist infection prevention in wound care
This is particularly important for post-surgical and chronic wounds.

In addition to moisture balance, adopting safe wound care practices to prevent infections further enhances healing outcomes.
4. Less Scarring and Better Skin Repair
When tissue dries out, scarring may become more noticeable.
Moist wound healing:
- Maintains tissue flexibility
- Supports smoother skin regeneration
- Improves cosmetic outcomes
This is beneficial for both medical recovery and aesthetic healing.
5. Natural Removal of Dead Tissue (Autolytic Debridement)
Moisture supports the body’s natural ability to break down and remove dead tissue.
This process:
- Promotes healthy tissue growth
- Reduces the need for manual cleaning
- Supports chronic wound management
How Moist Wound Healing Supports Recovery
Moisture-retentive dressings create an ideal healing environment by:
- Maintaining stable temperature
- Supporting new tissue formation
- Encouraging healthy blood circulation
- Preserving growth factors and healing proteins
This environment aligns with global medical wound management protocols and modern clinical practices supported by organizations such as the World Health Organization.
Choosing the Right Dressing for Moist Wound Healing
Selecting the best dressing for wound healing depends on wound type, exudate level, and skin condition.
Hydrocolloid Dressings
- Maintain moisture balance
- Suitable for minor burns and light drainage wounds
Foam Dressings
- Absorb excess fluid
- Keep the wound moist
- Ideal for moderate to heavily draining wounds
Hydrogel Dressings
- Hydrate dry wounds
- Provide cooling relief
- Reduce pain and discomfort
Alginate Dressings
- Highly absorbent
- Suitable for heavy exudate wounds
Film Dressings
- Thin and transparent
- Protect superficial wounds and abrasions (Velfix T Film)
Wounds That Benefit from Moist Healing
1. Chronic Wounds
- Diabetic foot ulcers
- Pressure injuries
- Venous leg ulcers
2. Acute Wounds
- Surgical incisions
- Burns
- Traumatic injuries
3. Fragile Skin Conditions
- Pediatric wounds
- Elderly skin injuries
Moist healing protects delicate skin and reduces friction damage.
Common Misbeliefs About Moist Wound Healing
- Myth: Moist wounds cause infections.
- Fact: Proper wound dressings create a protective barrier that helps prevent contamination.
- Myth: Scabs help wounds heal faster.
- Fact: Scabs can slow healing by blocking new cell growth.
Tips for Effective Moist Wound Healing
- Choose dressings based on wound size and fluid level
- Change dressings as recommended
- Avoid excessive moisture around wound edges
- Monitor for redness, swelling, or unusual discharge
- Seek medical care for deep or chronic wounds
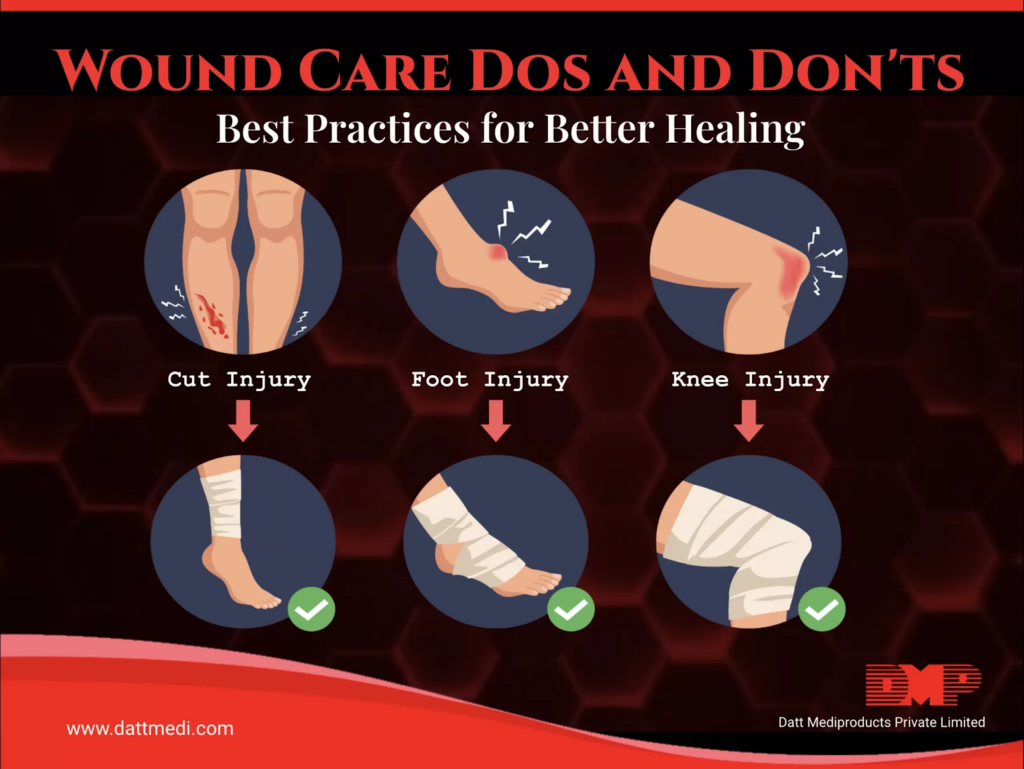
For more detailed guidance on wound care best practices — including cleaning, dressing changes, and monitoring — see our Best wound care practices for faster healing.
Challenges to Consider
Moist healing is highly effective, but improper use may cause complications:
- Excessive moisture may cause skin maceration
- Incorrect dressing selection can delay healing
- Increased susceptibility to infections and further damage
Guidance from healthcare professionals helps ensure safe and effective wound care and regular monitoring ensures optimal results
Evidence Supporting Moist Wound Healing
Clinical research shows moist wound environments can:
- Accelerate healing rates
- Reduce complications
- Improve skin regeneration
- Lower overall treatment costs
These benefits have made moist wound care a globally accepted standard supported by organizations such as the National Institute for Health and Care Excellence.
Studies indicate that wounds maintained in a moist environment may heal up to 40% faster compared to dry healing methods.
Moist wound healing has transformed modern wound care by enabling faster recovery, reducing discomfort, minimizing scarring, and improving overall healing outcomes. Using advanced wound care dressings helps maintain optimal moisture balance while protecting wounds from external contaminants.
For safe and effective healing, wound care decisions should always be guided by qualified healthcare professionals.






