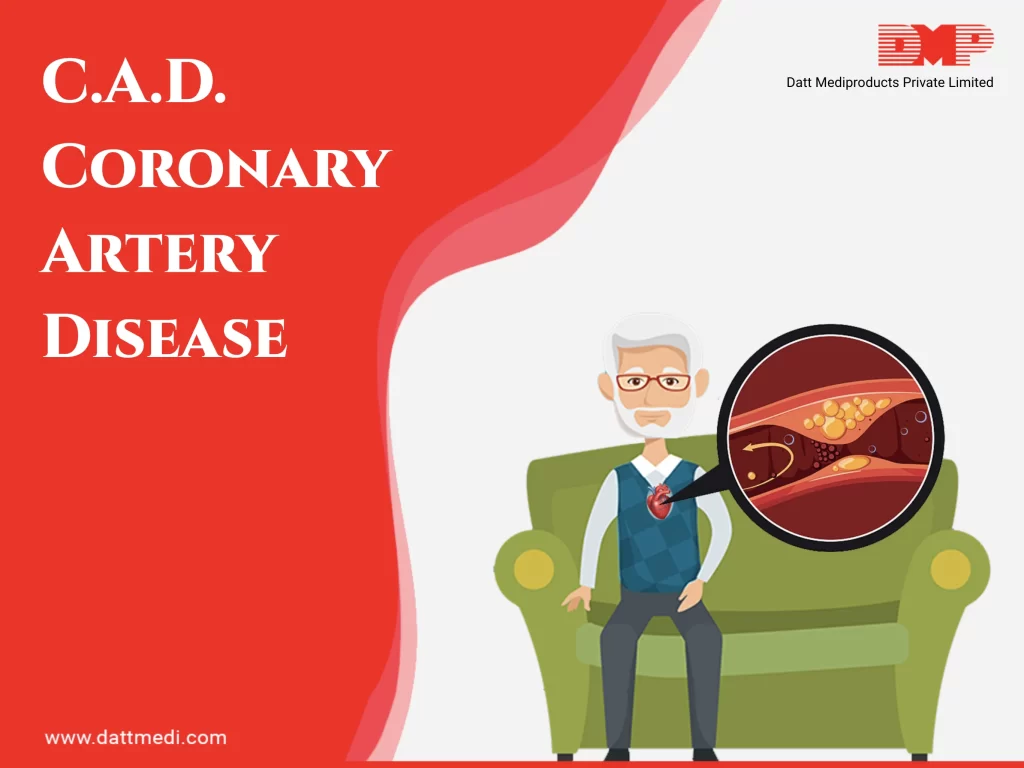
Our Heart is a muscular organ which pumps the blood to the other parts of the body. The Heart also requires the blood supply to function properly. Coronary artery disease develops when the blood vessel supplying blood to the heart “coronary artery” gets narrowed or a blockage occurs in it. This reduces the blood flow to the heart due to which the heart gets deprived of the oxygen and the essential nutrients for its working.
CAD can lead to a heart attack if the blood supply is completely stopped in one of the heart regions. Now let us understand what causes a Coronary Artery Disease.
Causes
CAD develops over the years. People won’t even know until symptoms develop. The fatty matter along with other substances like cellular wastes, cholesterol, proteins, etc. form PLAQUE on the inner walls of the arteries. As a result, the lumen of the arteries gets reduced resulting in bad blood flow to the heart.
Symptoms
- ANGINA: Angina is chest pain. An unusual pain, tightness, heaviness, and pressure felt in the chest usually on the middle or the left side. Angina can occur as a result of any emotional or physical stress and might stop after the stress is over. This pain might also spread to neck, shoulders, jaw, arms or back.
- DYSPNOEA: Dyspnoea is the shortness of breath. When our heart is not able to pump enough blood to the various organs, it causes extreme fatigue resulting in shortness of breath.
- HEART ATTACK: Also called as Myocardial Infarction, a Heart Attack occurs when the heart muscles don’t get enough oxygen resulting in the death of heart muscles. This happens when the blood supply to the heart muscles (coronary occlusion) is blocked by a clot called coronary thrombosis.
Prevention
People who smoke, have high cholesterol levels, high blood pressure, overweight, have a sedentary lifestyle, a poor diet, or have the family history are at a higher risk of developing the disease. Making a few lifestyle changes and reducing cholesterol levels can be a lot of help in preventing the disease.
Treatment
CAD can be treated with certain medications and Surgery.
- MEDICATIONS: Various types of medications can be used like:
1. Beta Blockers which help to reduce blood pressure
2. Nitroglycerin which helps to reduce the chest pain by widening the coronary arteries.
3. Angiotensin-converting enzyme (ACE) inhibitors which help to reduce blood pressure and slow the disease progression
4. Calcium channel blockers which help to reduce hypertension and increase the blood flow to the heart. - SURGERY: Surgery involves opening the blocked arteries. This can be done in various ways. Surgery is done if the patients don’t respond to the medications.
1. Coronary Artery Bypass Surgery: Cardiologist surgeon create a graft involving a blood vessel from any other part of the body to bypass the blocked artery.
2. Balloon Angioplasty and Stent Placement: This surgery involves inserting a catheter into the blocked artery following the insertion of a deflated balloon after which the balloon is inflated when it reaches the affected area. This causes breakage of the plaque. Balloon Angioplasty may be followed by placing a STENT which helps the artery to remain open.
3. Laser Surgery: Sometimes a laser surgery is performed involving making small holes in the heart muscle which might help to form new blood vessels.
We @ Datt Mediproducts recommend lifestyle changes and seeing a doctor immediately if anyone faces the CAD symptoms. A healthy diet accompanied by a regular exercise is a key to a healthy heart.