Managing Chronic Wounds in Diabetic Patients: Tips and Best Practices
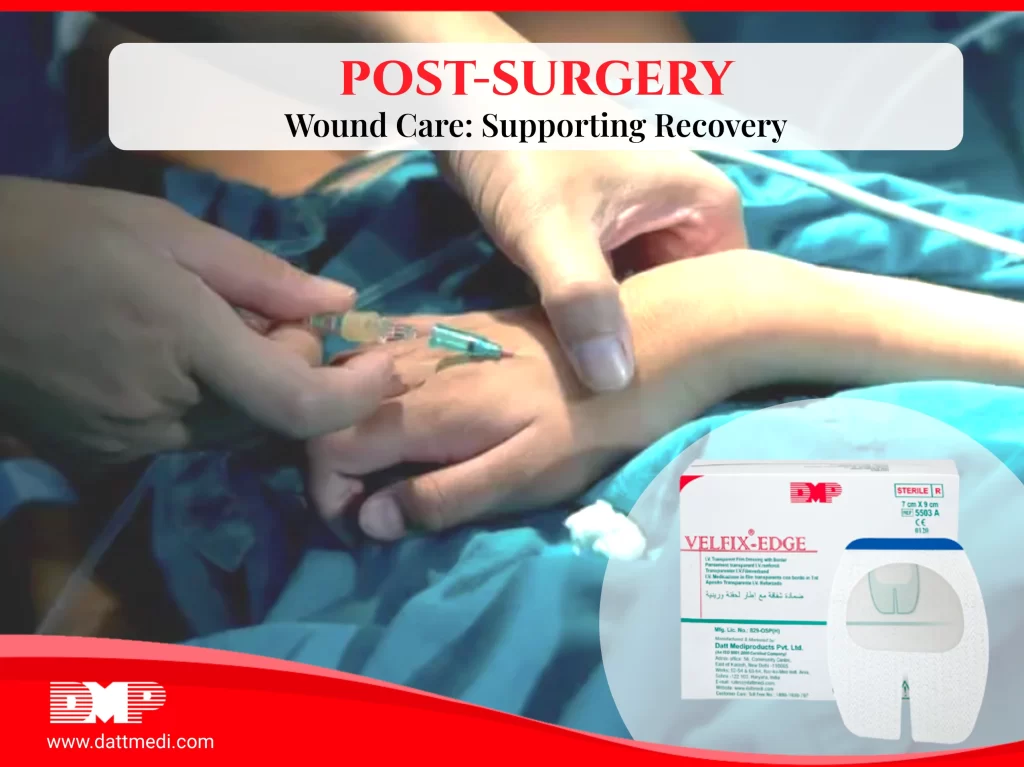
Chronic wounds, such as diabetic foot ulcers and pressure sores, pose a significant challenge to healthcare providers due to their resistance to healing. Factors such as poor circulation, diabetes, and malnutrition contribute to the delayed tissue regeneration seen in these wounds. This guide explores strategies to improve outcomes for diabetic patients dealing with chronic wounds.
Understanding Chronic Wounds
Chronic wounds develop and persist due to underlying systemic issues that impede natural healing. These include:
- Diabetic Foot Ulcers: Resulting from reduced blood flow and nerve damage, often on the feet.
- Pressure Sores (Bedsores): Caused by prolonged pressure on the skin, commonly in bedridden patients.
- Venous Leg Ulcers: Linked to chronic venous insufficiency, where blood flow back to the heart is impaired.
Example:
A diabetic foot ulcer might remain unhealed due to compromised blood circulation and nerve damage, requiring a tailored approach compared to pressure sores caused by external forces.
Selecting the Right Dressing
The choice of wound dressing plays a pivotal role in effective management:
- Hydrocolloid Dressings: Ideal for moderately exuding wounds; they absorb moisture, maintain a moist healing environment, and prevent infections. This makes them particularly effective for diabetic foot ulcers.
- Hydrogels: Suitable for dry wounds as they provide moisture to the wound bed, encouraging healing. However, they may not prevent infection and should be used in conjunction with appropriate infection control measures.
Infection Control: The Role of Antimicrobial Dressings
Chronic wounds are prone to infections that can hinder the healing process. Antimicrobial dressings play a crucial role in managing these infections and promoting recovery.
Introducing Velvert®, a natural-based patented antimicrobial formulation designed to address infection control in chronic wounds. Velvert® is broad-spectrum in nature, effectively combating all major superbugs and accelerating the wound healing process. Its advanced formulation is highly biocompatible, ensuring no side effects or contraindications, making it a safe and reliable choice for patients.
Example:
A pressure ulcer with a high risk of bacterial colonization benefits greatly from using Velvert®. Its broad-spectrum action not only reduces bacterial load but also creates an optimal healing environment, leading to faster recovery and improved patient outcomes.
Managing Exudate Levels
Excess moisture or dryness can impede wound healing. Dressing selection must align with the wound’s exudate level:
- Foam Dressings: Effective for heavily exuding wounds due to their superior absorption capabilities.
- Hydrocolloid Dressings: Suitable for wounds with moderate exudate, maintaining moisture balance without risking maceration.
Foam vs. Hydrocolloid for Heavy Exudate
Foam dressings are the preferred choice for high-exudate wounds as they prevent saturation and maceration. Hydrocolloid dressings may become overwhelmed, compromising the wound’s healing environment.
Nutritional and Lifestyle Interventions
Healing chronic wounds requires addressing systemic factors, including nutrition and blood glucose management:
- Nutrition: Adequate intake of vitamins A, C, zinc, and protein supports tissue regeneration and immune function.
- Glucose Control: Poor glucose control in diabetic patients delays healing. Maintaining optimal levels is essential for recovery.
For instance, a diabetic patient consuming a nutrient-rich diet while effectively managing their glucose levels is more likely to experience faster wound healing.
Continuous Monitoring and Expert Care
Regular assessment by healthcare professionals is essential for chronic wound management. Adjustments to treatment plans based on wound progress ensure the best outcomes. Starting with antimicrobial dressings often sets the foundation for successful healing without the need to switch to standard dressings.
Chronic wounds in diabetic patients demand a multifaceted approach that includes selecting the right dressings, managing infections and exudate, and addressing systemic factors such as nutrition and glucose control. By following these best practices, healthcare providers can significantly improve healing outcomes, reduce complications, and enhance the quality of life for patients.
At Datt Mediproducts, we are committed to delivering next-generation wound care solutions that prioritize patient comfort and clinical efficacy. Our range of advanced dressings, including gauze-based, film, post-operative, and antimicrobial options, is designed to cater to diverse wound management needs. Explore our comprehensive portfolio and discover how we can support your wound care journey.