Velvert®: Natural Antimicrobial Barrier Dressing effectively kills 99.9999% bacteria present in the wound.
Have you ever encountered a wound which doesn’t heal fast, where it takes weeks to heal? Have you thought it could be due to infection? Infections can halt the wound healing process as they prevent healthy tissue regeneration.
Different strains of bacteria delay the wound healing process in different ways. Some extend the inflammatory phase and others can interfere with the clotting mechanisms causing the wound to bleed continuously.
Various strains of bacteria have been documented for their notorious activities in delaying the healing process. A 2010 study published in the Journal of Dental Research shows that pseudomonas aeruginosa and staphylococcus are the two most damaging strains of bacteria.
We @ Datt Mediproducts Pvt. Ltd. introduce a novel patented natural anti-microbial barrier dressing “VELVERT®” which speeds up the healing process by effectively killing the microbes (99.9999%) present in the wound.
VELVERT® consists of a polymeric sponge loaded with patented natural antimicrobial formulations. All the components of the formulation work in a synergistic manner to achieve the reduction of microbial flora and enhance wound healing. VELVERT® is found to be effective even against most resistant Superbugs.
NOVEL FEATURES:
1. VELVERT® is a sponge based natural antimicrobial barrier dressing
b. The product is broad-spectrum in nature and effective against both gram-positive and gram-negative bacteria and also against various superbugs, some of which are listed below:
- Multi-drug resistant (MDR) Acinetobacter baumannii: Acinetobacter is most commonly associated with nosocomial infections and its infections lead to death in more than 50% cases. (Tuon et al., 2010b, 2011)
- Extended Spectrum Beta-Lactamase (ESBL): ESBL are the enzymes that cause resistance to most beta-lactam antibiotics, including penicillin, cephalosporins, and the monobactam aztreonam.
- New Delhi Metallo-beta-lactamase-1 (NDM-1): Superbugs with NDM-1 gene are resistant to even the strongest antibiotics.
- Methicillin-resistant Staphylococcus aureus (MRSA): These gram-positive bacteria are responsible for various difficult to treat infections in humans.
- Vancomycin-resistant enterococci (VRE): Enterococci lives in our intestines & vancomycin is the antibiotic used to treat the infections caused by this bacterium. When enterococci become resistant to the specific antibiotic, it becomes vancomycin-resistant enterococci. Most VRE infections originate in hospitals.
- Pseudomonas: People with a weakened immune system and those who have undergone surgery or are hospitalized are more vulnerable to pseudomonas infections. In such cases, the infection can be life-threatening.
2. The formulation is effective against superbugs, as proved in the Time Kill Assay, where the population of microorganisms is 99.9999 % reduced within 30 minutes.
3.. The zone of inhibition shows the antimicrobial activity of VELVERT®:
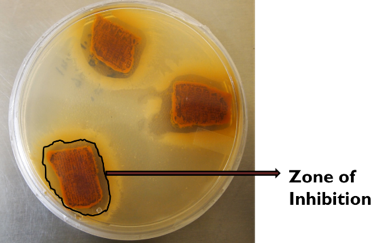
4. The dressing kills the microbes and enhances wound healing by increasing cell migration.
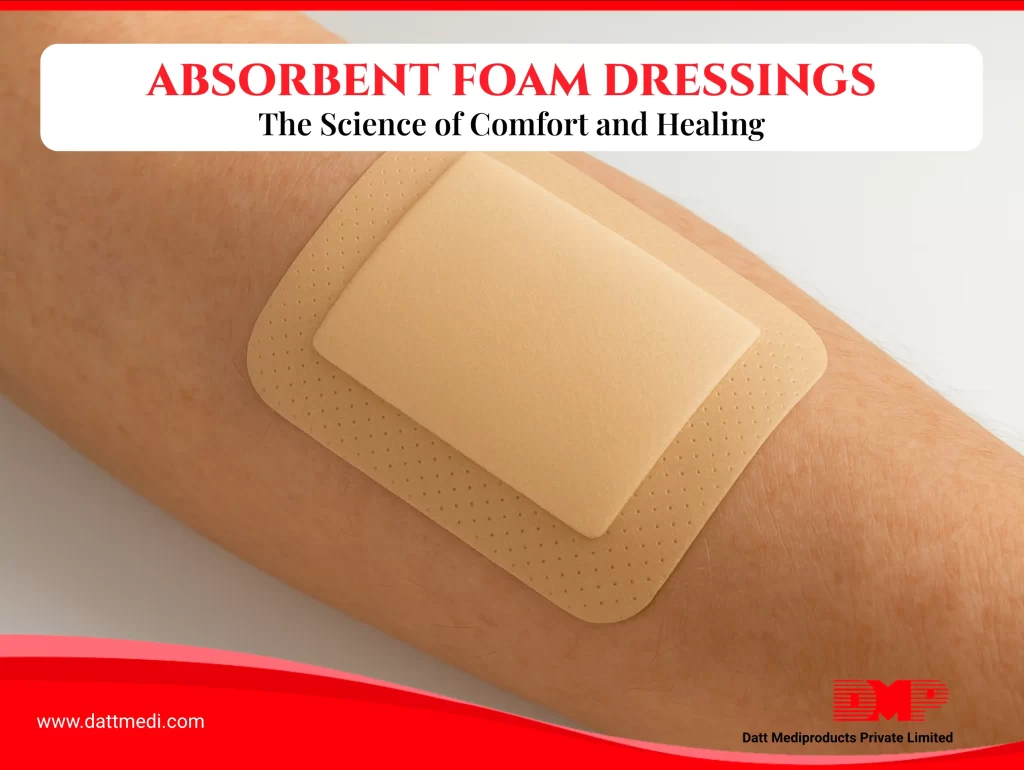
5. VELVERT® is highly porous in nature with a capacity to absorb exudates up to 18-20 times of its own weight and also aids in maintaining a moist wound environment.
6. The polymeric sponge is biocompatible and non-toxic to human tissue.
7. VELVERT® is soft and flexible, making it highly conformable for deep and irregular wounds.
VELVERT® reduces the microflora in wounds and actively promotes healing by stimulating stem cells that are present even in deep wounds and enhance the migration of fibroblast and keratinocytes and secretion of growth factors. VELVERT® is indicated as an antimicrobial barrier dressing for the management of partial- and full-thickness wounds for up to 5 days.
These wounds include:
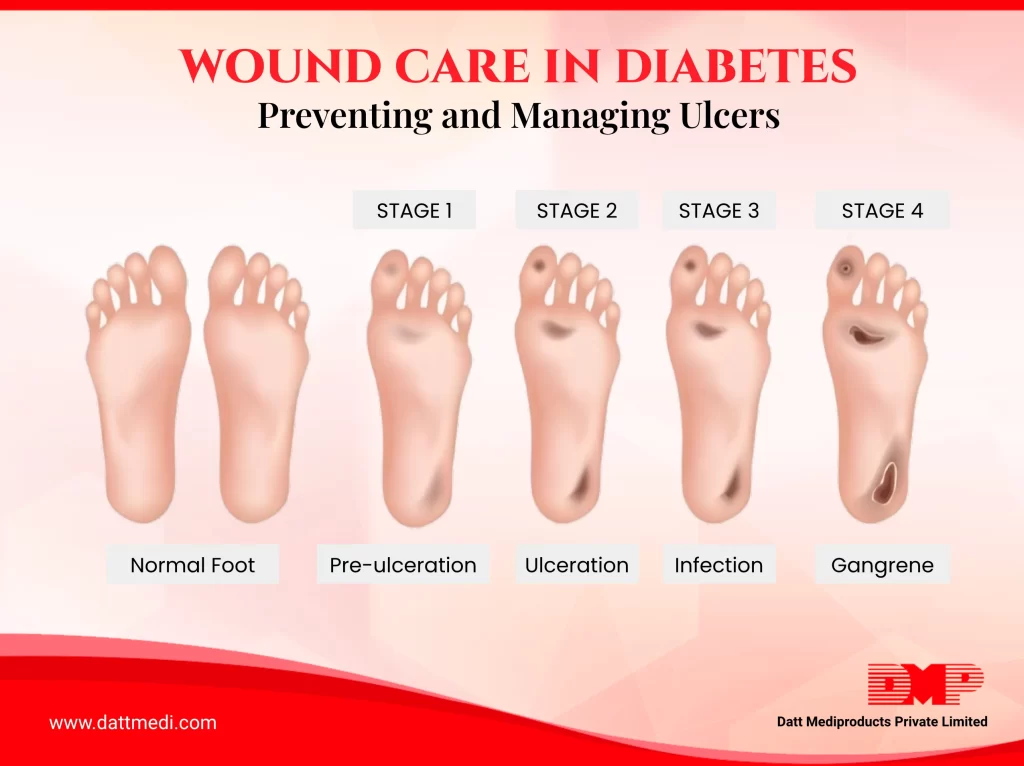
- Diabetic Foot Ulcers
- Skin Ulcers
- Pressure ulcers
- Venous ulcers
- Infected Wounds
- Skin grafting (donor sites)
- To cover grafts/dermal substitutes
- Catheterization sites
- Partial & full-thickness burn wounds
- Traumatic and surgical wounds
VELVERT® is also found to be effective in controlling central venous and arterial catheter insertion site infections.
Since the components in this product are from herbal/natural resources, VELVERT® can be changed very safely and eco-friendly and does not produce any adverse effect on the skin. Follow us @Datt Mediproducts to know more about such innovative patented products.