Discover Informative Blogs on Healthcare Solutions
Search by Blog
Read by Category
Patient Care Solutions
Health & Wellness
Environmental Health
First Aid & Emergency Care
Advance Wound Care
Wound Care
Your healing journey continues beyond this blog
Find the right products for better recovery at online store

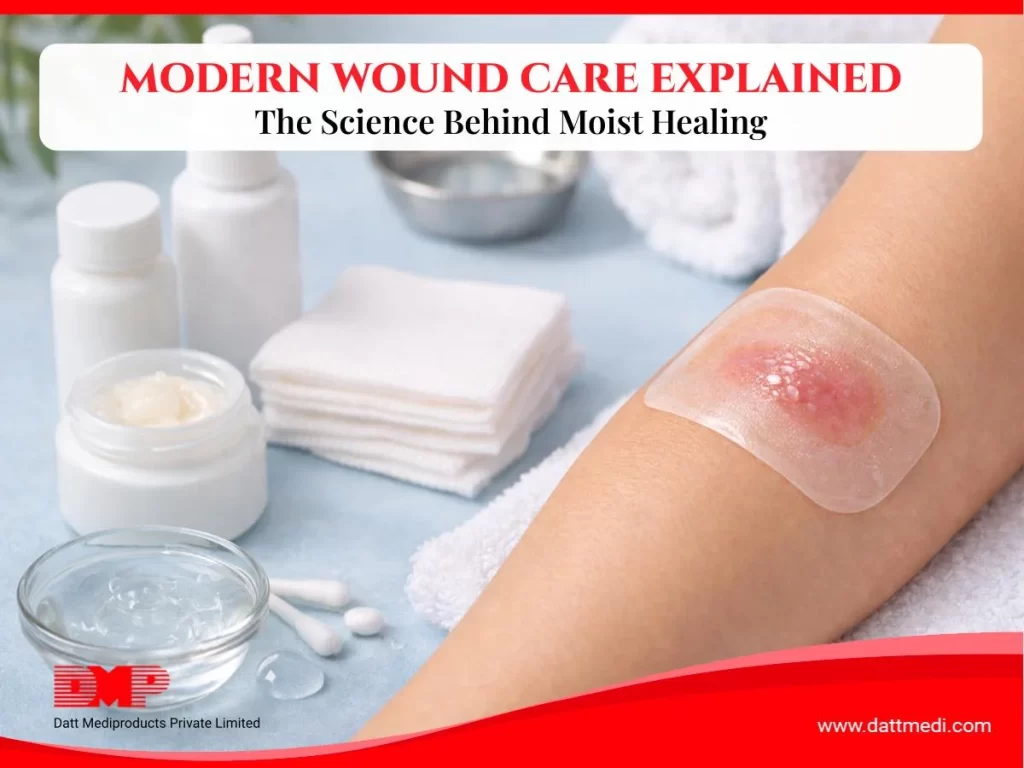
For many years, people believed that allowing a wound to dry out and form a scab was the best way to promote healing. Modern wound care science has shown that maintaining a moist healing environment can support faster tissue repair, reduce discomfort, and improve skin recovery.
Since its clinical adoption in the 1960s, moist wound healing has become a cornerstone of modern wound care in hospitals and home care settings worldwide. By protecting the wound and supporting the body’s natural repair process, this method helps improve healing outcomes and patient comfort.
What Is Moist Wound Healing?
Moist wound healing involves covering a wound with an advanced wound care dressing that maintains optimal moisture while protecting it from contaminants and bacteria.
Dry Healing Approach
- Allows a hard scab to form
- Can slow skin cell movement
- May delay tissue repair
Moist Healing Approach
- Keeps the wound hydrated
- Enables faster cell migration
- Supports efficient tissue regeneration
This balanced environment helps the body heal more effectively.
Moist Wound Healing vs Dry Healing: Key Differences
| Feature | Moist Healing | Dry Healing |
| Healing Speed | Faster | Slower |
| Pain Level | Reduced | Often higher |
| Infection Protection | Barrier protection | Exposure risk |
| Scarring | Less visible | More likely |
| Tissue Repair | Continuous | Interrupted by scab |
Why Moist Wound Healing Is Beneficial
1. Faster Healing
A moist environment allows skin cells to move easily across the wound surface.
- No hard scab blocking repair
- Continuous tissue rebuilding
- Shorter recovery time
This is especially beneficial for surgical wounds, burns, and chronic ulcers.
2. Reduced Pain and Discomfort
Dry wounds can expose nerve endings, increasing sensitivity and pain.
Moist dressings:
- Protect delicate tissue
- Reduce irritation
- Provide cushioning comfort
They are commonly used to soothe painful wounds and burns.
3. Lower Risk of Infection
Advanced wound dressings create a protective barrier against dirt and bacteria.
When combined with antimicrobial protection, they:
- Reduce contamination risk
- Support safer healing
- Assist infection prevention in wound care
This is particularly important for post-surgical and chronic wounds.

In addition to moisture balance, adopting safe wound care practices to prevent infections further enhances healing outcomes.
4. Less Scarring and Better Skin Repair
When tissue dries out, scarring may become more noticeable.
Moist wound healing:
- Maintains tissue flexibility
- Supports smoother skin regeneration
- Improves cosmetic outcomes
This is beneficial for both medical recovery and aesthetic healing.
5. Natural Removal of Dead Tissue (Autolytic Debridement)
Moisture supports the body’s natural ability to break down and remove dead tissue.
This process:
- Promotes healthy tissue growth
- Reduces the need for manual cleaning
- Supports chronic wound management
How Moist Wound Healing Supports Recovery
Moisture-retentive dressings create an ideal healing environment by:
- Maintaining stable temperature
- Supporting new tissue formation
- Encouraging healthy blood circulation
- Preserving growth factors and healing proteins
This environment aligns with global medical wound management protocols and modern clinical practices supported by organizations such as the World Health Organization.
Choosing the Right Dressing for Moist Wound Healing
Selecting the best dressing for wound healing depends on wound type, exudate level, and skin condition.
Hydrocolloid Dressings
- Maintain moisture balance
- Suitable for minor burns and light drainage wounds
Foam Dressings
- Absorb excess fluid
- Keep the wound moist
- Ideal for moderate to heavily draining wounds
Hydrogel Dressings
- Hydrate dry wounds
- Provide cooling relief
- Reduce pain and discomfort
Alginate Dressings
- Highly absorbent
- Suitable for heavy exudate wounds
Film Dressings
- Thin and transparent
- Protect superficial wounds and abrasions (Velfix T Film)
Wounds That Benefit from Moist Healing
1. Chronic Wounds
- Diabetic foot ulcers
- Pressure injuries
- Venous leg ulcers
2. Acute Wounds
- Surgical incisions
- Burns
- Traumatic injuries
3. Fragile Skin Conditions
- Pediatric wounds
- Elderly skin injuries
Moist healing protects delicate skin and reduces friction damage.
Common Misbeliefs About Moist Wound Healing
- Myth: Moist wounds cause infections.
- Fact: Proper wound dressings create a protective barrier that helps prevent contamination.
- Myth: Scabs help wounds heal faster.
- Fact: Scabs can slow healing by blocking new cell growth.
Tips for Effective Moist Wound Healing
- Choose dressings based on wound size and fluid level
- Change dressings as recommended
- Avoid excessive moisture around wound edges
- Monitor for redness, swelling, or unusual discharge
- Seek medical care for deep or chronic wounds
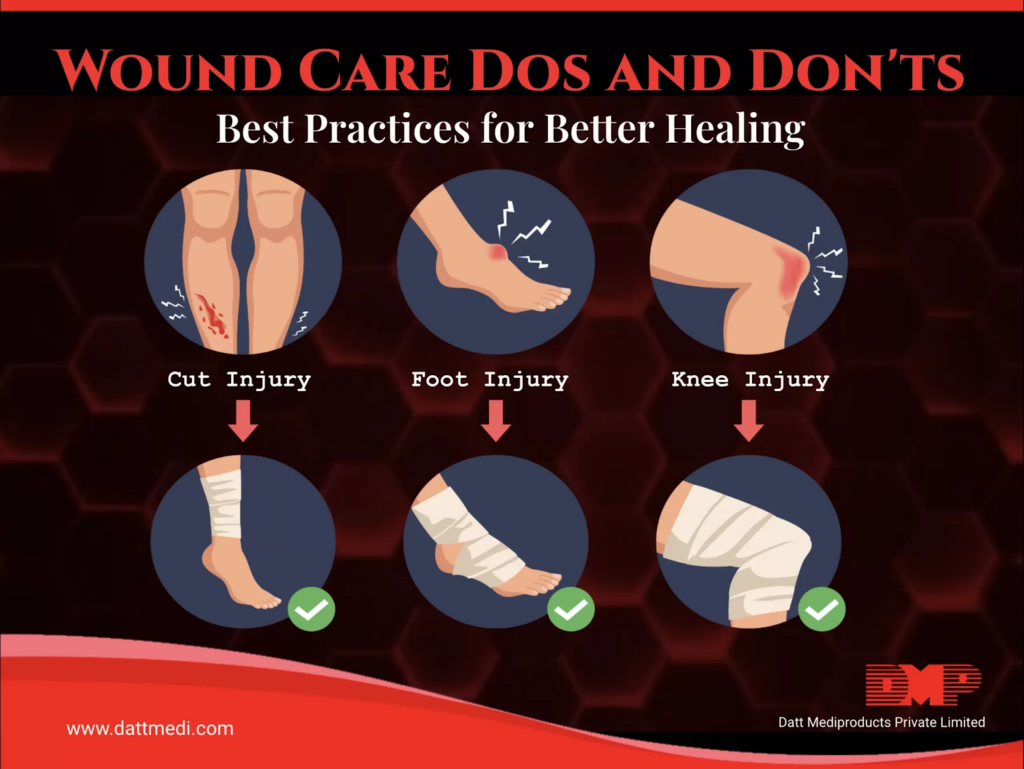
For more detailed guidance on wound care best practices — including cleaning, dressing changes, and monitoring — see our Best wound care practices for faster healing.
Challenges to Consider
Moist healing is highly effective, but improper use may cause complications:
- Excessive moisture may cause skin maceration
- Incorrect dressing selection can delay healing
- Increased susceptibility to infections and further damage
Guidance from healthcare professionals helps ensure safe and effective wound care and regular monitoring ensures optimal results
Evidence Supporting Moist Wound Healing
Clinical research shows moist wound environments can:
- Accelerate healing rates
- Reduce complications
- Improve skin regeneration
- Lower overall treatment costs
These benefits have made moist wound care a globally accepted standard supported by organizations such as the National Institute for Health and Care Excellence.
Studies indicate that wounds maintained in a moist environment may heal up to 40% faster compared to dry healing methods.
Moist wound healing has transformed modern wound care by enabling faster recovery, reducing discomfort, minimizing scarring, and improving overall healing outcomes. Using advanced wound care dressings helps maintain optimal moisture balance while protecting wounds from external contaminants.
For safe and effective healing, wound care decisions should always be guided by qualified healthcare professionals.
Introduction
Swelling in the legs or arms is more than a temporary discomfort. Persistent swelling can slow wound healing, limit mobility, and increase the risk of complications such as skin damage or venous ulcers.
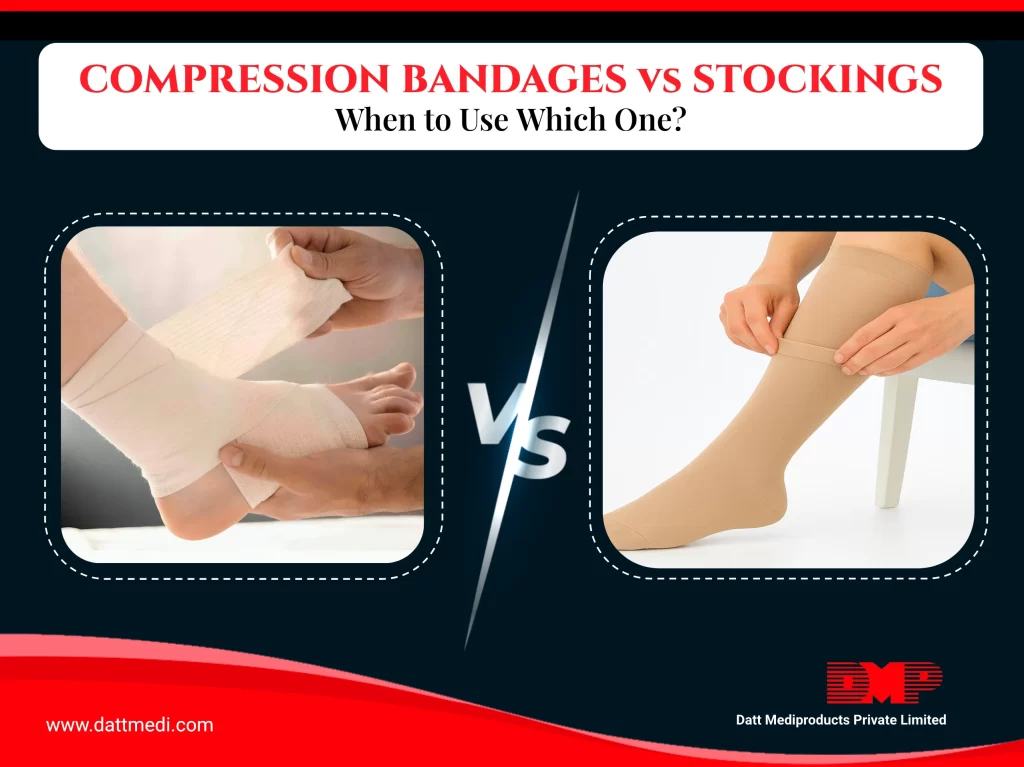
Compression therapy is a widely recommended medical approach used to support circulation and control fluid buildup in affected limbs. Among the most commonly used solutions are compression bandages and compression stockings. While both deliver controlled pressure to improve circulation, they serve different roles in treatment depending on the stage of recovery and the patient’s condition.
What Is Compression Therapy and Why Is It Important?
Compression therapy works by applying graduated pressure to a limb, helping blood and lymphatic fluid move back toward the heart. This controlled pressure reduces fluid accumulation in tissues and improves overall circulation.
Healthcare professionals commonly recommend compression therapy for conditions such as:
- Venous leg ulcers
- Varicose veins
- Lymphedema
- Post-surgical swelling
- Chronic venous insufficiency
- Injury-related edema
- Deep Vein Thrombosis
- Phlebitis
When used correctly, compression therapy helps reduce swelling, protect skin integrity, and support faster recovery.
Compression Bandages: Flexible Support for Changing Conditions
Compression bandages are stretchable wraps applied around the affected limb to provide controlled pressure. Because they can be adjusted during application, they are particularly useful when swelling levels change or when wounds require regular monitoring.
Types of Compression Bandages
- Short-Stretch Bandages : Short-stretch bandages provide limited elasticity and generate higher pressure when muscles move. This makes them suitable for patients who remain active, as muscle movement enhances the compression effect and supports venous return.
- Long-Stretch Bandages : Long-stretch bandages offer greater elasticity and maintain consistent pressure even when the limb is at rest. They are often used for patients with limited mobility or those recovering from surgery.
When Compression Bandages Are Commonly Used
Compression bandages are commonly recommended when treatment needs to adapt to changing conditions, including:
- Sudden or severe swelling
- Open wounds requiring wound dressings
- Post-surgical swelling management
- Limbs with irregular or changing shape
Their adjustability allows healthcare providers to modify pressure levels as swelling decreases and healing progresses.
Looking for reliable and adjustable compression bandages for effective therapy?

Explore our Compression Bandage here: View Product
Compression Stockings: Consistent Support for Long-Term Care
Compression stockings are specially designed medical garments worn like socks or sleeves. They apply graduated compression, with the highest pressure at the ankle that gradually decreases toward the calf or thigh.
This pressure pattern supports natural blood flow and helps prevent fluid from collecting in the lower limbs.
Compression Levels in Stockings
Medical compression stockings are available in different pressure strengths depending on treatment needs:
- Mild compression – Helps prevent early swelling and leg fatigue
- Moderate compression – Supports varicose veins and mild circulation problems
- Higher compression levels– Used for chronic venous conditions or post-ulcer management
When Compression Stockings Are Typically Used
Compression stockings are typically introduced after swelling has stabilized and the limb size becomes consistent.
They are commonly used for:
- Long-term swelling management
- Ongoing support for circulation disorders
- Prevention of venous ulcer recurrence
- Daily compression therapy for chronic conditions
Because they are easier to wear independently, stockings often improve treatment adherence for long-term care.

Explore our medical-grade Velcare Varicose Vein Stockings designed for effective compression therapy: View Product
Comparing Compression Bandages and Compression Stockings
| Feature | Compression Bandages | Compression Stockings |
| Flexibility | Highly adjustable | Fixed compression level |
| Best Stage of Treatment | Early or active treatment | Long-term maintenance |
| Ease of Use | Requires trained application | Easy for self-use |
| Wound Compatibility | Suitable for wound dressings | Usually used after wounds heal |
| Comfort for Daily Wear | Moderate | High |
| Adaptability to Swelling | Excellent | Limited |
When Are Compression Bandages the Better Choice?
Compression bandages Compression bandages are generally recommended during the initial stage of treatment, especially when swelling is unstable or wounds are present.
They are most suitable when:
- Swelling changes frequently
- Limb shape is uneven
- Wound dressings require regular replacement
- Compression pressure must be adjusted
Because they can be re-applied and modified, bandages allow clinicians to closely manage swelling while protecting healing tissues.
When Are Compression Stockings More Suitable?
Compression stockings are commonly used after the treatment phase once swelling has been reduced and limb size stabilizes.
They are ideal for:
- Long-term compression therapy
- Preventing recurrence of swelling
- Supporting circulation in chronic venous disorders
- Providing comfortable daily compression support
Regular use of properly fitted stockings helps maintain results achieved during earlier treatment.
Why Professional Guidance Matters
Selecting the right compression therapy requires careful assessment of several factors, including circulation health, wound condition, skin sensitivity, and patient mobility.
Incorrect compression levels or poorly fitted products can reduce treatment effectiveness and cause discomfort. Healthcare professionals ensure the correct compression type, pressure level, and fitting method are used for each patient.
Medical compression products manufactured under internationally recognized standards such as ISO and CE certifications further support safety, performance, and reliability in clinical and homecare environments.
Compression therapy plays an important role in managing swelling, supporting circulation, and improving wound healing outcomes.
Compression bandages offer flexibility during the active treatment stage, allowing healthcare professionals to adjust pressure as swelling changes. Compression stockings provide consistent and convenient compression for long-term management, helping patients maintain recovery and prevent future complications.
Understanding the differences between compression bandages and compression stockings enables more effective treatment decisions and supports better long-term vascular and wound care management.
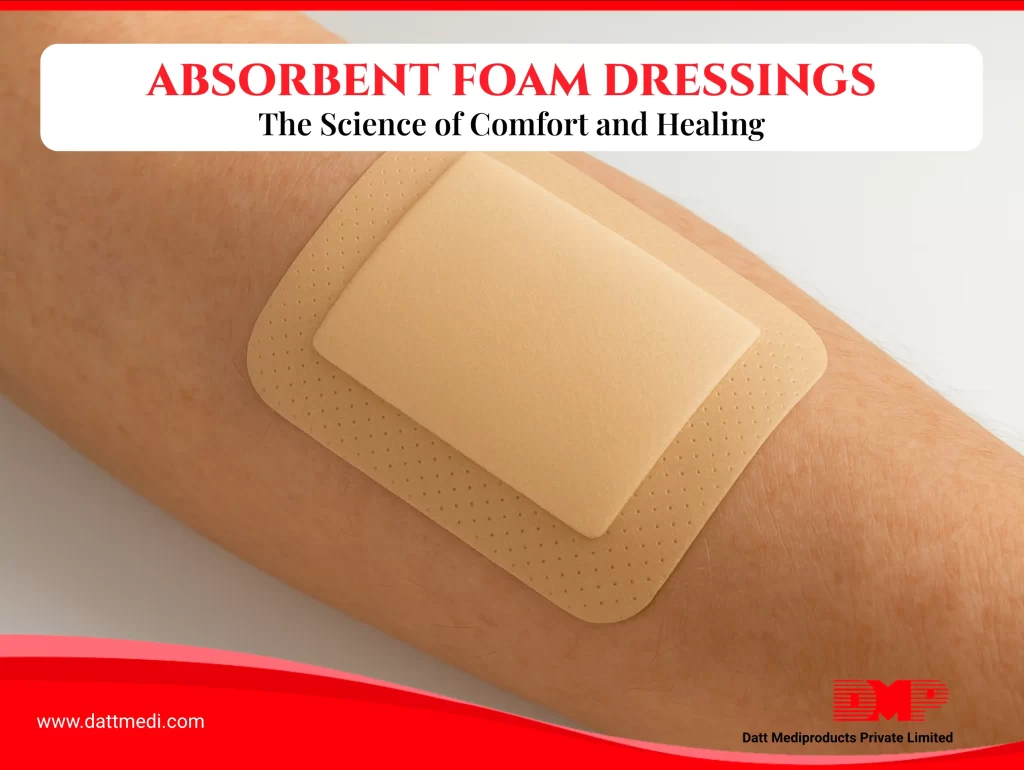
Absorbent foam dressings are advanced wound care solutions specifically designed to manage moderate to heavy wound exudate while maintaining a moist healing environment.
Maintaining the right moisture balance is critical for wound healing. Excess fluid can cause maceration and delay recovery, while insufficient moisture may slow tissue regeneration. Foam dressings are engineered to maintain this balance—supporting safer, more efficient healing across acute and chronic wound types.
Widely used in hospitals, long-term care facilities, and home-care settings, absorbent foam dressings are a core component of modern wound management protocols.
Clinical Overview: Absorbent Foam Dressings
- Designed for moderate to heavy exudate
- Maintain a controlled moist wound environment
- Reduce risk of periwound maceration
- Provide cushioning and mechanical protection
- Support atraumatic dressing removal
- Suitable for pressure ulcers, diabetic foot ulcers, venous leg ulcers, and surgical wounds
What Are Absorbent Foam Dressings?
Absorbent foam dressings are multi-layer wound dressings typically made from polyurethane foam. They are engineered to:
- Absorb and retain moderate to heavy wound fluid
- Protect surrounding skin from excess moisture
- Provide thermal insulation and cushioning
- Maintain optimal moisture levels for tissue repair
They are widely used in advanced wound care settings where effective exudate control and periwound protection are essential.
Why foam dressings are used
Wounds that produce fluid need balance—not dryness, not pooling moisture. Foam dressings maintain this balance, which supports natural tissue repair.
How they are built
- A highly absorbent foam layer that draws in and holds wound fluid
- A protective outer layer that allows airflow but blocks bacteria and external moisture
- Optional adhesive borders for secure placement without extra fixation
Foam dressings are widely used in acute care, long-term wound management, and post-surgical recovery across global healthcare systems, especially in wound care settings.
How Absorbent Foam Dressings Work
1. Managing Moderate to Heavy Wound Exudate
Foam dressings absorb excess fluid and lock it inside the dressing.
Why this matters:
Uncontrolled fluid can soften surrounding skin, increase leakage, and slow healing.
How it helps healing:
By keeping the wound surface balanced—not wet, not dry—foam dressings create conditions where new tissue forms more efficiently. Products such as Velnext® Foam Dressing are designed for this purpose.
2. Maintaining a Stable Healing Environment
While absorbing excess fluid, foam dressings preserve gentle moisture at the wound surface.
Clinical benefit:
Stable moisture supports faster cell growth and reduces repeated tissue disruption caused by frequent dressing changes, which is especially important in chronic wounds managed with advanced foam dressings
3. Cushioning and Physical Protection
The soft foam structure absorbs pressure and reduces friction.
Especially useful for:
- Heels
- Sacral area
- Elbows
- Other pressure-prone or mobile body parts
This protection helps prevent further tissue damage during daily movement and is a key benefit of foam-based wound dressings.

Read More about : VELFIX-S: Foam Dressings in Wound Care
Key Benefits of Absorbent Foam Dressings
Protects Periwound Skin
By preventing fluid leakage and excessive moisture accumulation, foam dressings reduce the risk of maceration and surrounding skin breakdown.
Enhances Patient Comfort
The flexible, conformable structure minimizes pain during wear and dressing removal, especially in chronic wound management.
Reduces Dressing Change Frequency
Due to their high absorbency, foam dressings can often remain in place for several days (subject to clinical assessment), improving patient compliance and care efficiency.
Supports Infection Management
In wounds with elevated infection risk, antimicrobial silver foam dressings may help manage bacterial load. These are typically used when clinical signs of infection are present or when risk factors exist.
Types of Absorbent Foam Dressings
Adhesive Foam Dressings
- Integrated fixation border
- Easy application
- Suitable for ambulatory patients and post-operative care
Non-Adhesive Foam Dressings
- Gentle on fragile or sensitive skin
- Require secondary fixation
- Ideal for elderly patients or delicate wound sites
Antimicrobial Foam Dressings
- Contain antimicrobial agents
- Support bacterial load management
- Used in infected or high-risk wounds
Foam Dressings vs Other Dressing Types
| Dressing Type | Best For | Not Suitable For |
| Foam Dressings | Moderate–heavy exudate | Dry wounds |
| Hydrocolloids | Light–moderate exudate | Heavily exuding wounds |
| Alginates | Heavy exudate or bleeding | Dry wounds |
| Transparent Films | Superficial wounds | Moderate–heavy exudate |
Selecting the appropriate dressing depends on wound characteristics, fluid level, and clinical assessment.
Ideal Wound Types for Foam Dressings
Absorbent foam dressings are commonly recommended for:
- Pressure ulcers
- Diabetic foot ulcers
- Venous leg ulcers
- Post-surgical wounds
- Traumatic injuries
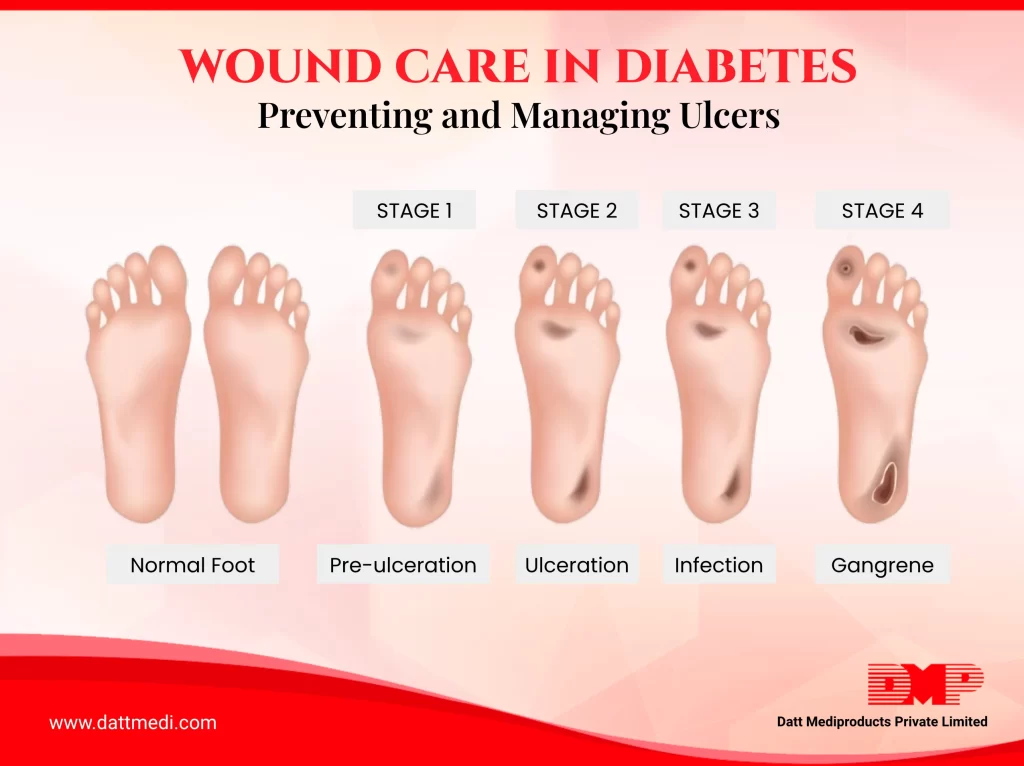
Read More: Proven Ways to Prevent Complications
Their ability to absorb fluid while protecting tissue makes them a reliable option for both acute and chronic wound care, including hospital-grade wound management.
When Foam Dressings May Not Be Appropriate
Foam dressings may not be suitable for:
- Dry or minimally exuding wounds
- Hard necrotic tissue or dry scabs
- Wounds requiring active debridement
In such cases, alternative dressing categories that donate moisture or facilitate debridement may be more appropriate based on professional evaluation.
Quality Standards and Clinical Reliability
High-performance absorbent foam dressings are manufactured in accordance with internationally recognized quality and safety standards, including ISO 13485 and CE certification.
As a manufacturer of certified advanced wound care solutions, DMP designs foam dressings aligned with global clinical standards, ensuring product reliability, patient safety, and consistent performance across healthcare environments.
Absorbent foam dressings combine smart material design with practical wound care needs. By controlling wound fluid, protecting fragile skin, and improving comfort, they play a vital role in modern wound management.
Selecting the right foam dressing—based on wound type, fluid level, and patient needs—can significantly improve healing outcomes and overall care quality.

Knowing how to clean a wound properly and apply the right dressing plays a critical role in healing outcomes. Inadequate wound care is one of the most common reasons wounds become infected or take longer to heal.
Whether managing a minor cut at home, caring for a surgical incision, or supporting chronic wound recovery, following evidence-based wound care practices helps protect the skin, reduce complications, and support natural tissue repair.
Why Proper Wound Care Is Important
Proper wound care involves cleaning the wound, protecting it with an appropriate dressing made from clinically tested materials, and regularly monitoring the healing progress.
Effective wound care:
- Reduces microbial contamination
- Minimizes inflammation and tissue damage
- Lowers the risk of scarring and delayed healing
- Supports tissue regeneration, especially in patients with diabetes, poor circulation, or reduced immunity
Maintaining a clean and protected wound environment allows new tissue to form safely and consistently.
Practical example:
Healthcare facilities worldwide follow standardized wound care protocols because consistent and correct wound management directly improves patient recovery outcomes.
Step-by-Step Guide: How to Clean a Wound
A. Prepare Before Cleaning the Wound
1. What to do:
Prepare yourself and gather supplies before touching the wound.
2. Why it matters:
Proper preparation minimizes the risk of introducing bacteria into the wound.
3. How to do it:
- Wash hands thoroughly and wear clean gloves.
- Keep sterile saline or clean water ready.
- Prepare clean, suitable wound dressings as advised, along with a waste disposal bag.
B. Clean the Wound Gently and Safely
1. What to do:
Remove visible dirt, debris, or dried discharge from the wound.
2. Why it matters:
Gentle cleaning reduces infection risk and supports faster healing.
3. How to do it:
- Rinse the wound using a mild soap and sterile saline or clean running water
- Use antiseptic solutions only if recommended by a healthcare professional
- Avoid alcohol or hydrogen peroxide directly on the wound, as these may damage healthy tissue and delay healing
C. Dry the Wound Area Carefully
1. What to do:
Dry the surrounding skin after cleaning.
2. Why it matters:
Excess moisture can weaken surrounding skin and slow healing.
3. How to do it:
- Gently pat the area dry using sterile gauze
- Avoid rubbing the wound surface
Choosing the Best Dressing for Open Wounds
A. Factors to Consider When Selecting a Dressing
The best dressing for open wounds depends on:
- Type of wound (minor cut, surgical incision, or chronic wound)
- Amount of wound exudate (fluid)
- Infection risk and patient activity level
Selecting the right dressing—based on wound type and healing needs—helps maintain an optimal wound environment and supports steady healing.
B. Common Types of Wound Dressings and Their Uses
- Gauze Dressings:
Suitable for minor wounds and short-term protection, such as Gamjee pads and cotton gauze rolls. - Foam Dressings:
Ideal for moderate to heavily exuding wounds, such as Velfix-S, which helps absorb excess exudate while maintaining a balanced wound environment. - Hydrocolloid or Hydrogel Dressings:
Help maintain a moist environment for healing. - Antimicrobial Dressings:
Recommended when infection risk is high or infection is present, such as Velvert, used under medical guidance.
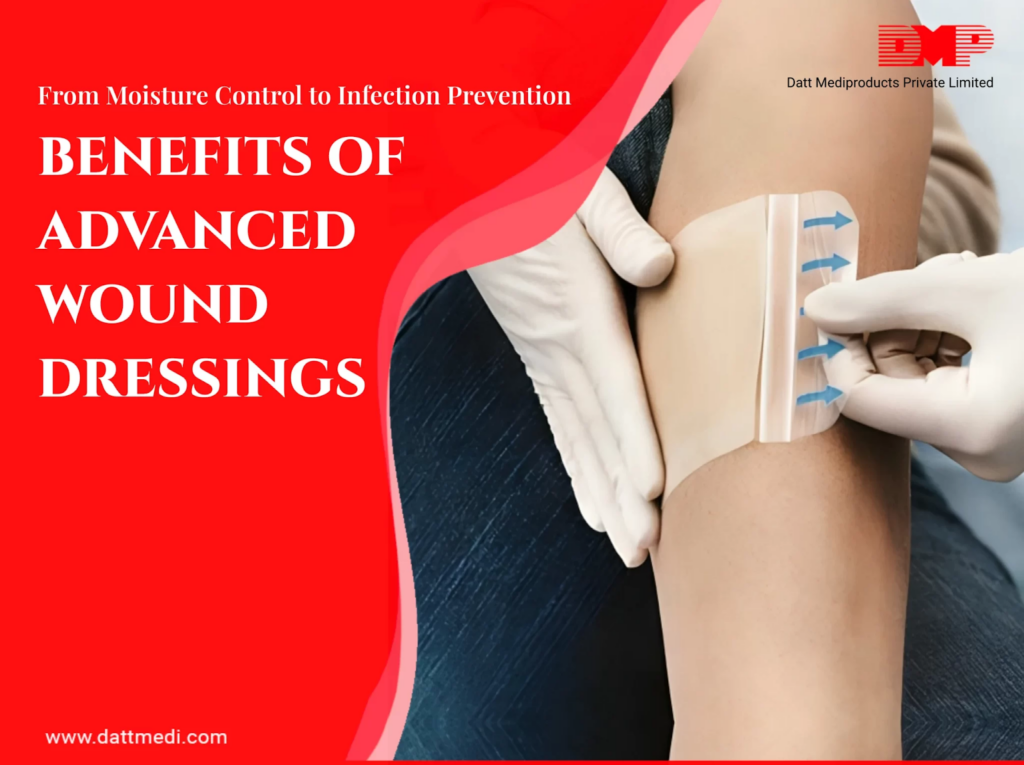
Modern wound management relies on advanced dressing technologies designed to maintain moisture balance and protect healing tissue. – Read More
How to Secure a Wound Dressing Correctly
1. Why it matters:
A dressing that is too loose may expose the wound, while one that is too tight can restrict circulation.
2. Best practices:
- Use transparent sterile film dressings (Velfix-T Film) to secure the primary dressing while allowing wound visibility.
- Medical adhesive tape may be used where appropriate.
- Ensure the dressing is secure, comfortable, and does not restrict blood flow.
How Often Should You Change a Wound Dressing?
Dressing change frequency depends on wound type, exudate level and medical advice. Change the dressing if:
- It becomes wet or contaminated
- There is increased redness, discharge, or odor
- Wounds with higher exudated will require more frequent dressing changes.
Regular dressing changes using clean and sterilized post-operative or wound dressings reduce infection risk and support faster healing.
Monitoring Wound Healing and Infection Signs
Check the wound daily for:
- Increased pain, redness, swelling, or warmth.
- Discharge or unusual odor (possible infected wound signs).
- Healthy pink or red tissue, which indicates healing.
If healing does not improve or symptoms worsen, consult a healthcare professional promptly.
If any warning signs persist or worsen, early identification is critical. Understanding the common symptoms of wound infection can help prevent serious complications and delayed healing.
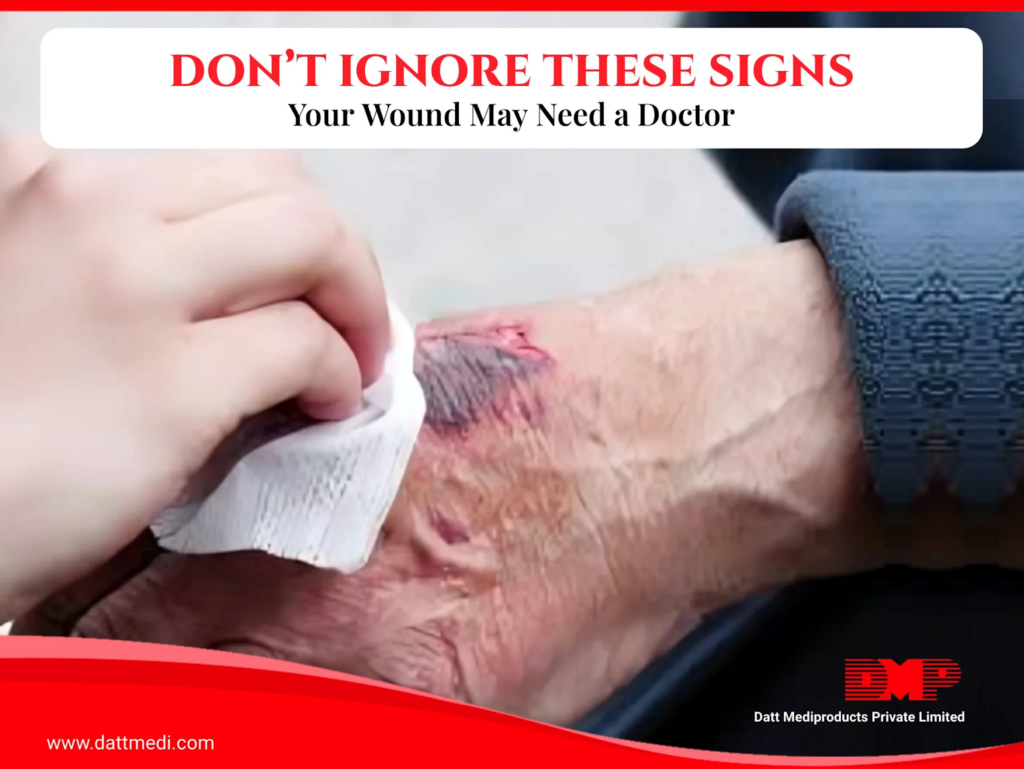
Read more: Signs of Infected Wounds: Symptoms, Risks, and When to Seek Medical Care
Common Wound Care Mistakes to Avoid
- Using non-sterile or unclean materials
- Leaving wounds uncovered for extended periods
- Reusing old or soiled dressings
- Applying products without professional advice
Avoiding these mistakes can significantly improve recovery outcomes.
When to Seek Medical Attention for a Wound
Seek professional care if:
- The wound is deep or bleeding heavily
- It is a burn
- Signs of infection are present
- The wound is chronic, such as diabetic foot ulcers or burns
- Healing does not progress over time
In such cases, specialized solutions like advanced wound dressings may be required, under the guidance of healthcare professionals.
Simple Tips to Support Faster Wound Healing
- Eat a balanced diet rich in protein, vitamins, and minerals
- Stay adequately hydrated
- Avoid smoking and excessive alcohol intake
- Get sufficient sleep to support tissue repair
Understanding how to clean a wound and apply the correct dressing is essential for safe and effective healing. By following approapriate wound care steps and using quality wound dressings manufactured under international standards such as ISO and CE, patients and caregivers can reduce complications and support better outcomes.
For complex or slow-healing wounds, timely medical guidance remains essential.
Medical Disclaimer
This content is intended for general wound care education and does not replace professional medical advice. Always consult a healthcare provider for serious, worsening, or non-healing wounds.

At-home wound care plays a bigger role in healing than most people realize. Many wounds that later become infected or heal slowly don’t start as serious injuries; they worsen because of small, everyday mistakes in home care.
These mistakes are rarely intentional. They usually occur due to confusion, over-cleaning, ignoring signs of infection or using unsuitable dressings. With the right approach, however, effective wound care at home can significantly reduce infection risk, improve comfort, and support faster healing.
This blog is especially helpful for individuals managing minor cuts, post-surgical wounds, or caring for elderly patients at home. It explains the most common at-home wound care mistakes, how to avoid them, and when professional medical help is necessary.
Common At-Home Wound Care Mistakes (And What Works Better)
1. Over-Cleaning the Wound
The Mistake
Cleaning the wound too frequently or using strong solutions such as spirit, iodine, or hydrogen peroxide.
Why This Is a Problem
While cleaning is essential, over-cleaning can damage newly forming tissue and slow the body’s natural healing process. Repeated use of harsh antiseptics may irritate the wound bed and delay recovery.
What to Do Instead
- Always wash your hand thoroughly first
- Clean once daily or if the dressing gets dirty
- Use a mild soap and clean water or saline
- Gently pat dry—do not scrub
Practical Insight
For most minor wounds, gentle cleaning combined with appropriate wound care dressings is sufficient to prevent infection and support healthy healing.
2. Touching the Wound or Dressing Surface
The Mistake
Directly touching the wound or the surface of the dressing that comes in contact with the skin.
Why This Increases Infection Risk
Hands naturally carry bacteria, even after washing. Touching sterile surfaces can transfer germs directly to the wound, increasing the risk of infection.
What to Do Instead
- Wash hands before and after wound care
- Handle dressings only from the edges
- Avoid reusing or adjusting used dressings
Practical Insight
Using sterile ready-to-use dressings helps maintain hygiene and reduces unnecessary handling during home care.
3. Using the Wrong Dressing for the Wound
The Mistake
Applying any available bandage without considering the wound type, size, or location.
Why This Slows Healing
An unsuitable dressing may stick to the wound, trap excess moisture, irritate surrounding skin, or restrict movement—leading to discomfort and delayed healing.
What to Do Instead
- Asses the wound.
- Depending on the type of wound choose an appropriate dressing. If you need help choosing a dressing or have any doubts of the type of wound please contact a healthcare professional.
- Choose sterile, breathable, non-irritating dressings
- Ensure secure but comfortable placement
- Change the dressing regularly and if it becomes wet, dirty, or loose
Practical Insight
Well-designed gauze-based dressings and post-operative film dressings support protection, comfort, and consistent healing at home.
Step-by-Step: Safe Wound Care at Home
Following a simple routine helps prevent infection and supports steady healing.
Step 1: Assess the wound
- Assess the wound to see how serious and what type of wound it is.
- You should seek professional care if:
- you can see the bone or blood vessels
- the bleeding doesn’t stop even after pressure is applied
- it is a burn wound
- it is a bite wound from an animal
Step 2: Prepare
- Wash hands thoroughly
- Keep all dressing materials ready
Step 3: Clean
- Rinse the wound gently with mild soap and clean water or saline
- Pat dry with sterile gauze such as cotton gauze products
Step 4: Dress
- If it is a minor cut of scrape let it air out, it doesn’t need a bandage
- For larger wounds apply a sterile dressing without touching the pad
- Smooth it gently so it stays in place
Step 5: Observe
- Check and clean the wound daily. Monitor for changes
- Replace the dressing as needed

For a more detailed look at everyday care practices that help wounds heal faster, see our wound care dos and don’ts for faster healing guide.

Warning Signs: When to Seek Medical Help
At-home wound care may not be enough if you notice:
- Increasing redness, swelling, or warmth
- Yellow or green discharge
- Persistent pain or fever
- A wound that does not improve after a few days
Early medical attention can prevent serious complications and support timely recovery.
Making At-Home Wound Care Safer and Simpler
Many households prefer sterile wound care solutions because they reduce guesswork and handling. These solutions are designed to:
- Support hygiene
- Reduce infection risk
- Simplify daily wound care routines
Such products are commonly used in hospitals and home-care settings and are manufactured following international quality standards such as ISO and CE, making them trusted across global healthcare markets.
Effective wound care at home is about balance—cleaning gently, protecting properly, and knowing when professional care is needed. By avoiding common mistakes and following simple, hygienic steps, healing outcomes can be significantly improved.
With the right approach and reliable advanced wound care products, healing at home can be safe, comfortable, and confident.
Medical Disclaimer
This content is intended for general wound care education and does not replace professional medical advice. Always consult a healthcare provider for serious, worsening, or non-healing wounds.

A well-fitted compression garment supports movement, reduces swelling, and improves overall comfort during recovery. Even small measurement errors can affect its effectiveness. Whether you are a patient, caregiver, clinician, or distributor, understanding how to measure compression garments correctly ensures safe therapy and reliable results.
For suitable options, check our Compression Stockings Collection.
1. Why the Right Measurement and Fit Matters
Compression garments apply controlled pressure along the limb. The correct size ensures even pressure distribution and therapeutic effectiveness.
Benefits of Proper Fit:
- Reduces swelling and discomfort
- Improves blood and lymph circulation
- Supports healing after injury, surgery, or chronic conditions
- Makes daily activities like walking, standing, or sitting more comfortable
Example: Someone managing mild swelling or early varicose veins often feels lighter and more supported when using a properly sized garment, following a reliable compression stocking size guide.
2. Tools You Need for Accurate Measurement
Accurate sizing doesn’t require advanced tools.
You need:
- A soft measuring tape
- Manufacturer’s compression measurement chart or sizing guide
- Notebook or phone to record values
- Mirror or assistance for hard-to-reach areas
- Good lighting for accurate readings
These simple tools help follow a medical compression garment sizing guide and reduce measurement errors.
3. Step-by-Step Guide: How to Measure Correctly
i) Ankle: Measure the narrowest point above the ankle bone.
ii) Calf: Measure the widest part of the calf for proper fit and support, including wide-calf users.
iii) Thigh (for thigh-high garments): Measure the thickest part of the thigh to avoid rolling and ensure secure fit.
Leg Length:
- Knee-high: heel to just below the knee crease
- Thigh-high: heel to the top of the thigh

iv) Arms (for sleeves/supports): Measure wrist, forearm, upper arm, and arm length. This ensures smooth, even compression from wrist to shoulder.
Quick Tips:
- Measure early in the morning when swelling is minimal.
- Sit comfortably, keep tape snug, measure twice, and avoid measuring over clothes.
4. Common Fitting Mistakes to Avoid
- Too Tight: Can cause numbness, tingling, or deep marks.
- Too Loose: Slipping or wrinkling reduces effectiveness.
- Incorrect Length: Too short rolls or digs in; too long bunches or slides down.
- Not Rechecking: Limb size changes due to swelling, healing, or weight changes—regular measurement is important.
For reference, see our Compression Stockings Size Chart India.

5. When to Consult a Healthcare Professional
Specialists can confirm the correct compression level and ensure measurements match your condition, especially after surgery or for vascular issues.
Consult if you notice:
- Persistent or increasing swelling
- Discomfort while wearing the garment
- Size falling between two chart options
- Post-surgical changes
- Conditions like diabetes or vascular disorders
Professional guidance ensures safe and effective therapy, particularly when using compression garments for varicose veins.
Accurate measurements are the foundation of effective compression therapy. Using simple tools, careful technique, and a trusted compression stocking size guide ensures your garment fits comfortably and supports healing. When unsure, consulting a healthcare professional provides confidence and safer results.

